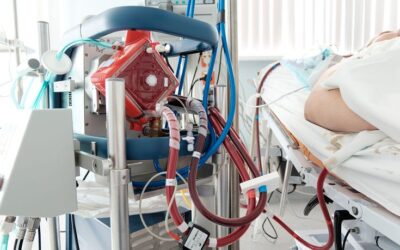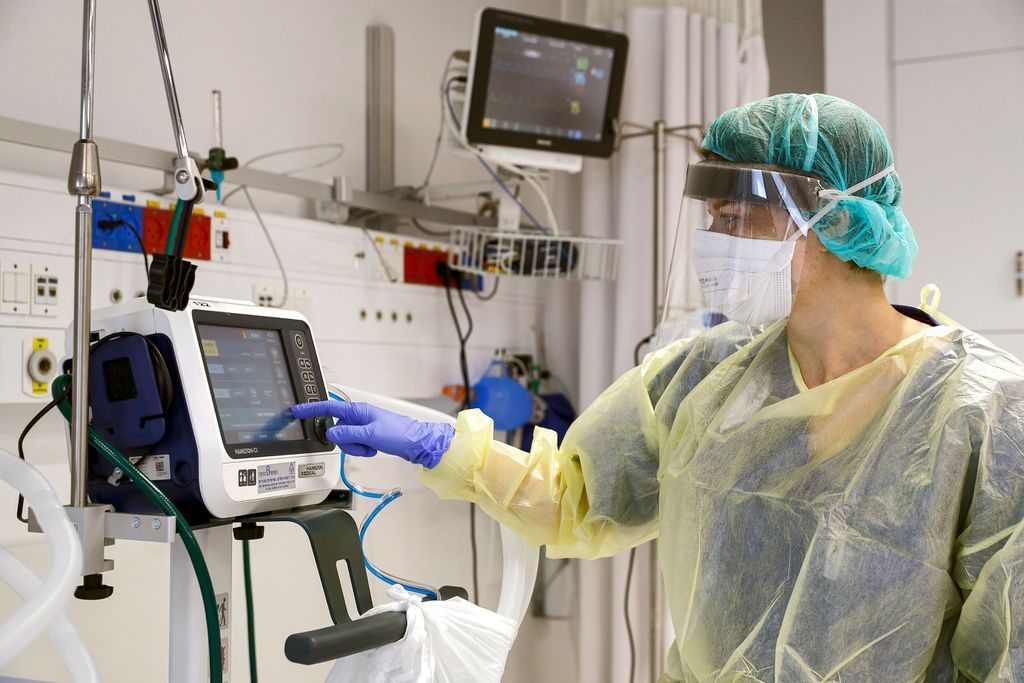
When a loved one is transferred to the Intensive Care Unit (ICU) and placed on a ventilator, it can be one of the most stressful and overwhelming moments for families. Mechanical ventilation — commonly referred to as “being on the ventilator” – is often surrounded by fear and misunderstanding. Many believe it means there is little hope of recovery or that it leads to permanent dependence.
In reality, ventilators are lifesaving machines designed to give critically ill patients a chance to survive and recover. This blog aims to separate myths from facts so families can better understand the purpose and process of mechanical ventilation.
Myth 1: Being Placed on a Ventilator Means There is No Hope
Fact:
Mechanical ventilation is not the end — it is the beginning of aggressive life support. Ventilators take over the work of breathing when the lungs are unable to do so adequately on their own due to pneumonia, ARDS (Acute Respiratory Distress Syndrome), severe trauma, or major surgery.
By ensuring adequate oxygen supply and removal of carbon dioxide, the ventilator gives the patient’s lungs time to rest and heal while doctors treat the underlying illness.
Myth 2: Ventilators are Painful and Uncomfortable
Fact:
Although a breathing tube (endotracheal tube) is required, it is inserted under anesthesia or sedation to keep the patient comfortable. Most patients are kept sedated in the early stages of mechanical ventilation to reduce pain, anxiety, and distress.
As recovery progresses, sedation is gradually reduced to allow the patient to start breathing partly on their own — an important step toward coming off the ventilator.
Myth 3: Once on a Ventilator, a Patient Cannot Come Off
Fact:
Across ICUs worldwide, most patients are successfully weaned off ventilators. The ICU team’s goal is always to remove the ventilator as soon as it is safe.
Weaning is a step-by-step process where ventilator support is gradually reduced until the patient’s lungs are strong enough to resume normal breathing. The decision depends on several factors, including the patient’s underlying condition, oxygen levels, breathing muscle strength, and overall progress.
Myth 4: Ventilators Do More Harm Than Good
Fact:
Modern ventilators are designed with advanced technology to protect the lungs. Intensivists, respiratory therapists, and nurses monitor ventilator settings continuously and adjust them as needed to minimize the risk of ventilator-induced lung injury.
Evidence-based protocols are followed to use the lowest safe pressures and volumes to avoid unnecessary strain on the lungs.
Myth 5: Patients on Ventilators Are Always Unconscious
Fact:
Not all ventilated patients are kept fully unconscious. Sedation levels are tailored to each patient’s needs. In some cases, patients can be awake, comfortable, and even communicate through gestures or writing.
Allowing patients to be partially awake, when safe, often helps with quicker recovery and faster weaning.
Myth 6: Ventilation Always Leads to Long-Term Dependence
Fact:
Long-term ventilator dependence is uncommon. It usually occurs only in patients with irreversible conditions such as advanced neuromuscular disorders or end-stage lung disease.
For most critically ill patients, ventilation is a temporary measure to support breathing until their lungs recover enough to work independently.
The Role of the Critical Care Team
Mechanical ventilation management is a highly specialized process requiring the combined expertise of intensivists, respiratory therapists, and critical care nurses. A skilled critical care physician such as Dr. Amit Kumar Choudhary plays a crucial role — from deciding when to initiate ventilation to adjusting settings and supervising the weaning process for the best possible outcome.
Families are encouraged to have open conversations with the ICU team about the patient’s condition, progress, and plan of care.
Conclusion
Mechanical ventilation is one of the most powerful tools in modern medicine. It is used to save lives when patients are critically ill and unable to breathe adequately on their own. Understanding how ventilators work and why they are used can help families feel more informed and reassured during an emotionally challenging time.
For expert management of patients requiring ventilator support, you can trust Dr. Amit Kumar Choudhary – Consultant Critical Care Medicine, Pune. His evidence-based approach and compassionate team ensure that every patient receives the highest standard of care during their most critical moments.