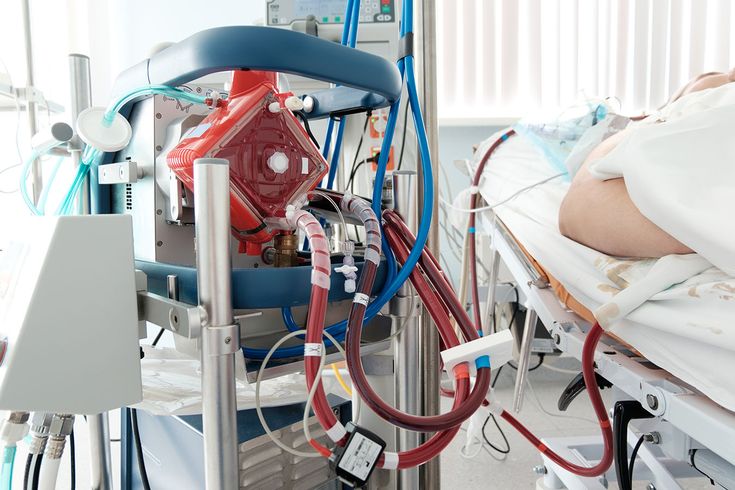
When a patient’s lungs or heart quit functioning in spite of maximum medical intervention, time itself is the most important aspect for saving their life. In life-threatening situations like these, physicians can resort to cutting-edge life support therapies that can “borrow” the function of these organs for a short while. The most astoundingly innovative innovation in contemporary critical care medicine is ECMO — Extracorporeal Membrane Oxygenation.
This life-saving technology has saved thousands of people around the globe, yet it remains poorly understood beyond intensive care units (ICUs). Let’s divide what ECMO is, when it is applied, and why it can be the difference between life and death.
What is ECMO?
ECMO is a specialized device that does the work of the heart and/or lungs outside the body. “Extracorporeal” is a term that means “outside the body,” and “membrane oxygenation” is the process of introducing oxygen and removing carbon dioxide from blood.
Simply put, ECMO removes the patient’s blood from the body, runs it through a man-made lung (oxygenator), and returns it to the body. This rests and recovers the heart and lungs while the machine keeps circulation and oxygenation going.
Types of ECMO
There are two principal types of ECMO utilized in critical care medicine:
- Veno-Arterial (VA-ECMO):
- This form supports heart and lung function. This is usually applied if the patient is in critical cardiogenic shock, cardiac arrest, or following major heart surgery when the heart cannot pump at its best.
- Veno-Venous (VV-ECMO):
- This form supports only lung function. It is usually applied for patients suffering from severe respiratory failure, such as ARDS (Acute Respiratory Distress Syndrome) or severe pneumonia, including due to influenza or COVID-19.
When is ECMO Used?
ECMO is not primary treatment. It is for people with severe heart or lung failure who have not gotten better with usual treatments such as ventilators, drugs, or other therapies. Some typical situations are:
- Severe ARDS: When the mechanical ventilation cannot provide sufficient oxygenation.
- Cardiogenic Shock: When the heart is unable to pump sufficient blood even after medication and other aids.
- Post-Cardiac Surgery Support: When the heart must have time to rest after extensive surgery.
- Massive Pulmonary Embolism or Severe Pneumonia: When oxygenation is severely compromised.
- Bridge to Transplant: In patients waiting for heart or lung transplantation.
How ECMO Saves Lives
The greatest benefit of ECMO is that it purchases precious time. By performing the work of compromised organs, ECMO provides an opportunity for the patient’s lungs and heart to recover while physicians address the underlying pathology. For instance, in viral pneumonia complicated by ARDS, ECMO can provide oxygenation while the lungs slowly recover from infection.
Various studies and global registries have demonstrated that ECMO can remarkably enhance survival rates in highly selected patients if applied at the appropriate time and in an appropriate environment. The success hinges on early detection, specialized team coordination, and timely activation.
Risks and Considerations
As with any complex medical treatment, ECMO carries risks. These consist of bleeding, infection, blood clotting, and cannula-related complications from catheters placed in large veins. Thus, ECMO must always be done in an ICU with a skilled multidisciplinary team that can closely observe and manage potential complications.
The Role of a Skilled Critical Care Physician
ECMO involves meticulous patient selection and exact management. A well-trained intensivist such as Dr. Amit Kumar Choudhary, with considerable experience in ECMO, CRRT, and high-level ICU care, is important in providing the best outcomes. From determining whether to start ECMO to directing an experienced team in the care of the patient, the skill of the attending physician directly influences survival and recovery.
Conclusion
ECMO is arguably one of the most sophisticated and life-saving devices in critical care medicine today. Though it is reserved for only the most extreme cases, its prompt use can mean the difference between death and survival.
If you or your loved one is experiencing a critical cardiac or respiratory emergency, seeking treatment from a hospital with ECMO centers and trained intensivists is crucial.
Dr. Amit Kumar Choudhary – Consultant Critical Care Medicine, Pune brings over a decade of experience in managing critically ill patients, including those requiring ECMO support. His commitment to evidence-based, patient-centered care ensures that patients receive the highest standard of treatment during the most critical moments of their lives.